Gujarat Board GSEB Textbook Solutions Class 11 Biology Chapter 17 Breathing and Exchange of Gases Textbook Questions and Answers.
Gujarat Board Textbook Solutions Class 11 Biology Chapter 17 Breathing and Exchange of Gases
GSEB Class 11 Biology Breathing and Exchange of Gases Text Book Questions and Answers
Question 1.
Define vital capacity. What is its significance?
Answer:
Vital capacity is the maximum volume of air a person can breathe in after a forced expiration. It is the sum of Inspiratory reserve volume (IRV), Expiratory reserve volume (ERV) and the Tidal volume (TV).
The vital capacity is different for a different person. Its higher in athletes than in non-athletes, in mountain dwellers than in people living on plains and in youth than in old age. Cigarette smoking reduces the vital capacity.
Question 2.
State the volume of air remaining in the lungs after a normal breathing.
Answer:
The volume of air remaining in the lungs even after a forcible expiration averages 1100mL to 1200 mL.
![]()
Question 3.
Diffusion of gases occurs in the alveolar region only and not in the other parts of the respiratory system. Why?
Answer:
Alveoli are the primary sites of the exchange of gases. The exchange of gases also occurs between blood and tissues. O2 and CO2 are exchanged in these sites by simple diffusion mainly based on pressure/concentration gradient. The solubility of the gases, as well as the thickness of the membranes involved in diffusion, are also some important factors that can affect the rate of diffusion.
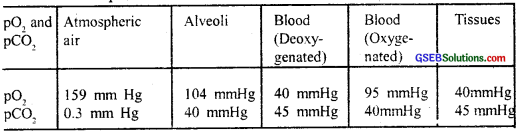
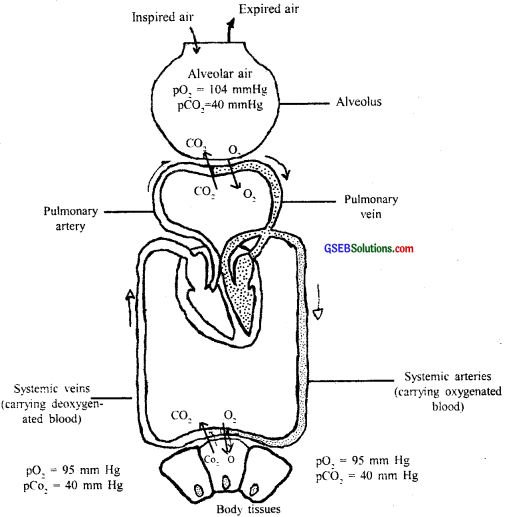
Pressure contributed by an individual gas in a mixture of gases is called partial pressure and is represented as pO2 for oxygen and pCO2 for carbon dioxide. Partial pressures of these two gases in the atmospheric air and the two sites of diffusion are given in Table 17.1 and in fig. 17.1. The data given in the table clearly indicates a concentration gradient for oxygen from alveoli to blood and blood to tissues. Similarly, a gradient is present for CO2 in the opposite direction i.e., from tissues to blood and blood to alveoli. As the solubility of CO2 is 20-25 times higher than that of O2, the amount of CO2 that can diffuse through the diffusion membrane per unit difference in partial pressure is much higher compared to that of O2.
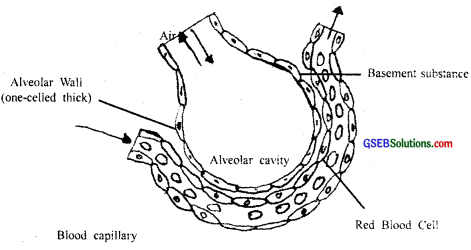
The diffusion membrane is made up of three major layers (fig. 17.2) namely, the thin squamous epithelium of alveoli, the endothelium of alveolar capillaries, and the basement substance in between them. However, its total thickness is much less than a millimeter. Therefore, all the factors in our body are favorable for the diffusion of O2 from alveoli to tissues and that of CO2 from tissues to alveoli. Table 17.1 Partial pressures of oxygen and carbon dioxide at different parts involved in diffusion in comparison to those in the atmosphere.
![]()
Question 4.
What are the major transport mechanisms for CO2? Explain
Answer:
Nearly 70% of CO2 is transported as bicarbonates.
(1) CO2 produced by the tissues, diffuses passively into the bloodstream and passes into RBCs. Here CO2 reacts with water to form carbonic acid. This reaction takes less than 1 second to complete
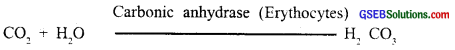
(2) Soon it dissociates into hydrogen and bicarbonate ions
![]()
(3) The oxyhemoglobin nbO2 of erythrocytes is acidic and remains in association with K+ ion as KHbO2
The H+ ion released from HCO2, combine with hemoglobin after its dissociation from the K+ ion.
![]()
Majority of HCO3– ion diffuses into plasma atom ∝ concentration gradient.
(4) HCO3 ion cambium with hemoglobin to form Haemoglobin acid (H-Hb)
![]()
(5) In response, Cl– ion diffuses from plasma into erythrocytes to maintain the ionic balance. This is called the chloride shift.
Question 5.
What will be the pO2 and pCO2 in the atmospheric air compared to those in the alveolar air?
- pO2 lesser, pCO2 higher
- pO2 higher, pCO2 lesser
- pO2 higher, pCO2 higher
- pO2 lesser, pCO2 lesser
Answer:
(1) Where there is low pO2 high pCO2, high H+ concentration and higher temperature exist, the conditions are favorable for dissociation of oxygen from the oxyhemoglobin.
(2) Where there is high pO2, low pCO2, lesser H+ concentration, and lesser temperature, the factors are all favorable for the formation of oxyhemoglobin whereas in the tissues.
(3) When pCO2, is high and pO2. is low as in the tissues, more binding of carbon dioxide occurs whereas.
(4) When the pCO2, is low and pO2, is high as in the alveoli, dissociation of CO2 from carbamino-hemoglobin takes place, i.e., CO2, which is bound to hemoglobin from the tissues is delivered at the alveoli.
![]()
Question 6.
Explain the process of inspiration under normal conditions.
Answer:
Inspiration can occur if the pressure within the lungs (intrapulmonary pressure) is less than the atmospheric pressure, i.e., there is a negative pressure in the lungs with respect to atmospheric pressure. Inspiration is initiated by the concentration of the diaphragm which increases the volume of the thoracic chamber in the anteroposterior axis.
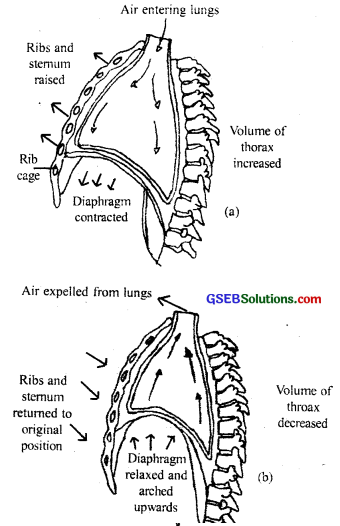
The contraction of external intercostal muscles lifts up the ribs and the sternum causing an increase in the volume of the thoracic chamber in the dorsoventral axis. The overall increase in thoracic volume causes a similar increase in pulmonary volume. An increase in pulmonary volume decreases the intrapulmonary pressure to less than the atmospheric pressure which forces the air from outside to move into the lungs, i.e., inspiration (fig 17.3a).
We have the ability to increase the strength of inspiration with the help of additional muscles in the abdomen. On average, a healthy human respires 12-16 times/minute. The volume of air involved in respiratory movements could be estimated by using a spirometer which helps in the clinical assessment of pulmonary functions.
![]()
Question 7.
How is respiration regulated?
Answer:
Human beings have a significant ability to maintain and moderate the respiratory rhythm to suit the demands of the body tissues. This is done by the neural system. A specialized center present in the medulla region of the brain called the respiratory rhythm center is primarily responsible for this regulation. Another center present in the pons regions of the brain called the pneumatic center can moderate the functions of the respiratory rhythm center. The neural signal from this center can reduce the duration of inspiration and thereby after the respiratory rate. A chemosensitive area is situated adjacent to the rhythm center which is highly sensitive to CO2 and hydrogen ions.
An increase in these substances can activate this center, which in turn can signal the rhythm center to make necessary adjustments in the respiratory process by which these substances can be eliminated. Receptors associated with the aortic arch and carotid artery also can recognize changes in CO2 and H+ concentration and send necessary signals to the rhythm center for remedial actions. The role of oxygen in the regulation of respiratory rhythm is quite insignificant.
Question 8.
What is the effect of pCO2 on oxygen transport?
Answer:
Partial pressure of CO2, hydrogen ion concentration and temperature are the factors that regulates binding of O2 with haemoglobin to form oxyhaemogiobin. In the alveoli, there is high PO2 low PCO2, lesser H+ concentration and lower temperature that favours the formation of oxyhaemogiobin. In the tissues, there is low PO2, high PCO2, high H+ concentration and higher temperature that favour the dissociation of oxygen from the oxyhemoglobin.
![]()
Question 9.
What happens to the respiratory process in a man going up a hill?
Answer:
At a hill (high altitude) the pressure of air falls and the person cannot get enough oxygen in the lungs for diffusion. blood. Due to insufficient O2, the person has difficulty breathing at high altitudes. The person feels difficulty such as breathlessness, headache, dizziness, irritability, nausea, vomiting, mental fatigue, and a blush tongue on the skin, nails, and lips.
Question 10.
What is the site of gaseous exchange in an insect?
Answer:
Insects have a network of tubes (tracheal tubes) to transport air within the body. Air enters the spiracles during inspiration and reaches the tracheoles which contain tissue fluids. Oxygen in the air dissolves in those fluids and reaches the cells.
![]()
Question 11.
Define oxygen dissociation curve. Can you suggest any reason for its sigmoidal pattern?
Answer:
A sigmoid curve is obtained when the percentage saturation of hemoglobin with O2, is plotted against the PO2. This curve is called the oxygen dissociation curve and is highly useful in studying the effect of factors like pCO2, H+ concentration, etc., on the binding of O2 with hemoglobin.
Each hemoglobin molecule can carry a maximum of four molecules of O2 binding of oxygen with hemoglobin. It is primarily related to the partial pressure of O2, The partial pressure of CO2, hydrogen ion concentration, and temperature are the other factors that can interfere with this binding.
Question 12.
Have you heard about hypoxia? Try to gather information about it, and discuss it with your friends.
Answer:
Hypoxia is the condition in which there is a deficiency of oxygen at the tissue level.
- Arterial hypoxia: It’s because of low level of oxygen in the blood. It occurs when the atmosphere does not contain enough oxygen and there is an obstruction in the respiratory passage.
- Anaemic hypoxia: It is due to very low level of haemoglobin in the blood.
- Stagnant hypoxia: It is due to the inadequate blood flow to deliver oxygen to the tissue.
- Historic hypoxia: It is due to the presence of toxic substances in the oxygen inhaled, e.g.: Cyanide poisoning.
Question 13.
Distinguish between
- IRV and ERV
- Inspiratory capacity and Expiratory capacity
- Vital capacity and Total lung capacity
Answer:
(1) IRV and ERV
Inspiratory Reserve volume IRV:
The additional volume of air, a person can inspire by a forcible inspiration. This averages 2500 ml to 3000 ml.
Expiratory Reserve Volume ERV:
With the additional volume of air, a person can expire by a forcible expiration. This averages 1000 ml to 1100 ml.
(2) Inspiratory capacity and Expiratory capacity
Inspiratory capacity:
The total volume of air a person can inspire after a normal expiration. This includes tidal volume and inspiratory reserve volume (TV + IRV).
Expiratory capacity:
The total volume of air a person can expire after a normal inspiration. This includes tidal volume and expiratory reserve volume (TV + ERV).
(2) Vital capacity and Total lung capacity
Vital capacity:
The maximum volume of air a person can breathe in after forced expiration. This includes ERV, TV, and IRV or the maximum volume of air a person can breathe out after a forced inspiration
Total lung capacity:
The total volume of air accommodated in the lungs at the end of forced inspiration. This includes RV. ERV, TV, and IRV or vital capacity + residual volume.
![]()
Question 14.
What is Tidal volume? Find out the Tidal volume (approximate value) for a healthy human in an hour.
Answer:
Tidal volume is the volume of air inspired or expired during normal respiration. It is approximately 500 ML. A healthy man can inspire or expire approximately 360 L to 480 L of air every hour.